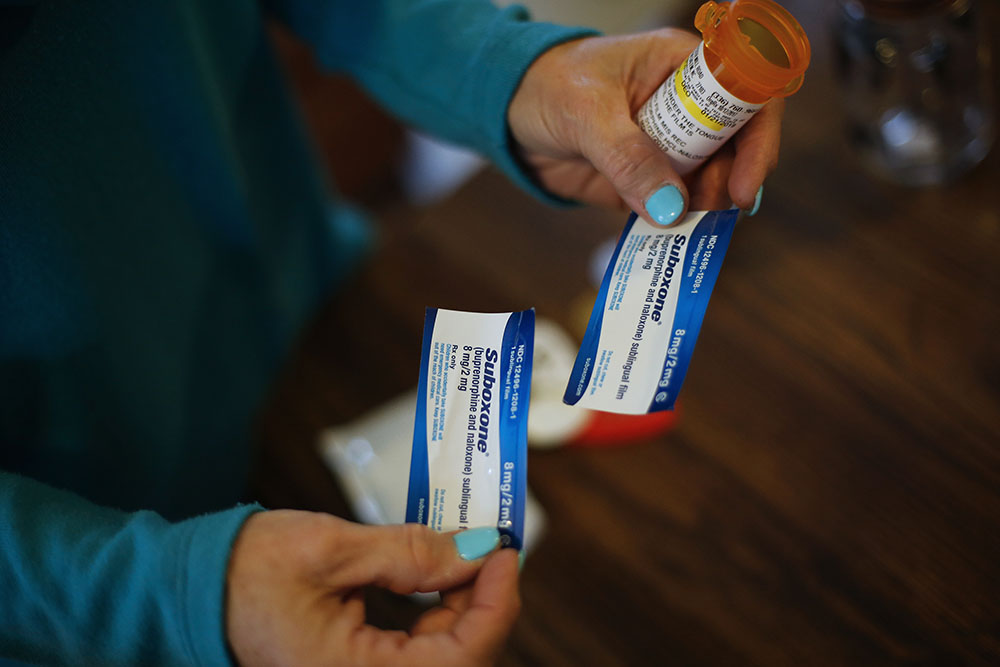
I just watched my husband run out the door. Not straight to his job as a cook, since his restaurant is shut down during the pandemic, but to his opioid treatment provider—a facility legally allowed to dispense methadone for the treatment of opioid addiction—so he can get his daily dose before the doors close for the day.
He still has to go every single day to get his medication, without which he would go into weeks of painful opioid withdrawal. My husband is one of hundreds of thousands of people across the country who rely on medications like methadone and buprenorphine to curb addiction to opioids and stay out of withdrawal, and who are now wondering whether they are going to continue to have access during the novel coronavirus pandemic, or risk being exposed to the virus by visiting facilities daily.
Get Talk Poverty In Your Inbox
The short answer is yes, facilities that prescribe and dispense these medications are continuing to run, and patients should not lose access to medications for opioid use disorder during this crisis. Methadone and buprenorphine are classified by the World Health Organization as essential medicines, which means continued access to them should be a priority. Various government agencies have issued guidelines and legal exceptions to a number of rules and regulations that usually limit access to these medications, in the hope of reducing visits to clinics.
But, of course, there’s a longer and far more complex answer as well.
Although methadone and buprenorphine treat the same disorder in relatively similar ways, they are governed by vastly different sets of rules and regulations. “On the [buprenorphine] side, the minimum you tend to see prescribed is a week. It would be easy in that case to give those patients a two-week prescription or call in an extra script with a refill. On the [methadone] side, that’s where it gets hairy,” said Zac Talbott, president of the National Alliance for Medication Assisted Recovery (NAMA-R), who also has direct experience as a patient and running facilities that provide these medicines.
Buprenorphine can be prescribed by any doctor or advanced practice registered nurse who has taken an eight-hour waiver course. That means patients can access it in a number of settings including primary care, psychiatry, gynecology, or addiction treatment facilities. Methadone, on the other hand, can only be dispensed for addiction treatment from a licensed opioid treatment provider (OTP), commonly referred to as a methadone clinic. It is governed by a complex web of rules, regulations, and policies that come from federal agencies, state authorities, and individual clinic directors. Since methadone is a better option for people with higher tolerances to opioids, and doesn’t require patients to go into withdrawal before starting it, it’s essential that both medicines are available.
“There’s going to be a broad variety in the way OTPs respond,” said Talbott. “Patients need to realize this could vary from state to state because of state authorities.”
Across the nation, State Opioid Treatment Authorities, who make state-level decisions about medications for opioid use disorder, have been looking to the federal Substance Abuse and Mental Health Services Administration (SAMHSA), for guidance on how they can respond to the novel coronavirus outbreak. This agency governs the rules around making medication available to be taken at home, instead of in a clinic (colloquially called “takehomes”), and many other methadone regulations at the federal level. Elinore F. McCance-Katz, the head of SAMHSA and the assistant secretary for mental health and substance use, told TalkPoverty by email that “SAMHSA/HHS are working in an ongoing manner with states and communities facing these issues. We have provided flexibilities to the states to help to assure that those on medications for opioid use disorders continue to get their medication. We have also been working to expand the ability to provide services by telehealth modalities wherever possible.”
Washington state, where the first confirmed cases of COVID-19 appeared in the United States, was the first state to receive the ability to dispense extended takehomes, lasting up to 14 days, to specified populations without first applying for individual permissions like providers must do normally.
“As of the 9th we have essentially put out seven different types of blanket takehome exception requests that programs can request per federal law to allow a large majority of individuals who are considered stable—and that’s determined at the discretion of each program medical director—to allow them to move beyond just daily or close to daily dosing,” said Jessica Blouse, of the Washington State Opioid Treatment Authority. “For buprenorphine there are no federal rules, so [those patients] can be moved to whatever level can be determined as safe.”
But that doesn’t mean all Washington patients will receive these benefits. Tanna, a patient who lives between the cities of Seattle and Tacoma, said she has not been offered any takehome doses. The reason, she was told, is because she has been with that provider just over three months, so she is still considered a new and therefore unstable patient—even though she transferred from another clinic where she had earned a month of takehomes.
She is also required to attend four hours of group therapy each month. Last week, her group had eight attendees and she did not notice any special precautions in place due to the virus.
“The only accommodation they’ve made [in the clinic] is at the dosing window there’s now hand sanitizer, the trash is moved a little bit, nurses wear gloves, and the [dosing] window screen is lowered,” she said.
On March 16, SAMHSA updated its guidelines specifying that all states with declared states of emergency could request blanket exceptions in order to provide stable patients with 28 days of takehome medication, and 14 days of takehome medication for patients considered less stable but still able to safely handle the extra medication. In states without a declared emergency status, each clinic is eligible to apply for similar exceptions for their patients.
The updated guidelines from SAMHSA allow states and providers greater flexibility to dispense takehome medication—but that does not mean that every clinic will utilize that flexibility to its fullest extent, nor that they will apply it to each patient.
“It may come down to the fact that patients will need to be given 14 day supplies,” said Mark Parrino, president of the American Association for the Treatment of Opioid Dependence. “However it should be case by case …We want to let people quarantine to clearly stop the spread of the disease, [but] remember we are dealing with opioids. Opioids in the hands of unstable patients can be dangerous. We don’t want to flood the community with a lot of methadone in the hands of unstable patients who may not be able to deal with the fact that suddenly they have a two-week supply.”
“People who are least likely to get takehomes are people who are new to treatment and people who have unstable housing, unstable psychosocial situations, people who might be continuing to use other substances, people with underlying health concerns; things that mean they have instability in their life. I would argue they are the people who should get takehomes immediately,” said Keith Brown, a harm reduction advocate currently working at the county level in Schenectady, New York on the COVID-19 response. “This is going to get into the argument about which is more dangerous, giving people takehomes they might sell or whatever—but in a public health crisis, people are going to have to make determinations about what makes sense. Having a few hundred people come into a clinic every day is a transmission nightmare.”
It’s impossible to know what every single state and clinic will do with their expanded discretion. Reports coming in from patients and providers indicate the response is as varied as opinions on addiction.
Justine Waldman, the medical director of REACH, a harm reduction-based buprenorphine clinic in Ithaca, New York, has begun offering one and two month scripts to her buprenorphine patients, giving longer scripts to those who have a harder time getting in to the office or who have a history of missing appointments. Her emphasis is on access and patient health over surveillance. The caveat, she stressed, is that this is an entirely new situation that is evolving each day.
“We might decide tomorrow that the way we’re doing it now isn’t working. We are really having to come together and take it day by day,” she said.
Jana Burson, who is the medical director of an OTP in North Carolina, said that while her clinic is not giving most patients extended takehomes, they are utilizing measures to help keep the facility sanitized, and to enforce social distancing while patients are in the building. For example, the lobby chairs have been spaced to be at least six feet apart, and some counselors with smaller offices are moving individual counseling sessions to larger rooms. They are aggressively disinfecting chairs, door handles, countertops, and other shared surfaces.
Vanessa, a patient in North Carolina, reported that her clinic was not dispensing any extra takehomes. She normally receives takehomes for Saturday, Sunday, and Monday, but was called in this Monday for a drug test and bottle check, a practice observed by some clinics in which they count patients’ takehome bottles. She described her clinic as “really business as usual” besides seeing staff taking patient temperatures. She noted that her temperature was not taken when she stopped by for the drug test. On Thursday morning she texted me an update that she was going to be given seven takehomes, but would have to pay for them out of pocket.
Stephanie, a patient in Pennsylvania, says she has continued to receive her regular six takehomes, but that group meetings and individual counseling sessions have been canceled until further notice. When she pressed for more information, her counselor replied that for the clinic to shut down “it would have to be the end of the world and there would be zombies,” but conceded that they were giving some extra takehomes to medically fragile patients.
Emily, who has hepatitis C, has not been offered any takehome doses by her Lexington, Ky., clinic, but reported that all patients are being stopped upon entering the building and questioned about potential symptoms. People who report feeling unwell are dosed from their cars, and only five patients are being allowed to enter the building at a time. Groups have been canceled, and individual counseling sessions are being done over the phone.
Samantha, a pregnant patient in Central Florida, reported that she was given 13 takehomes and had a doctor’s appointment canceled so she would not have to go in on an extra day.
In South Florida, my husband Ricardo still goes in for dosing every day, but told me his clinic was advising patients to be prepared to pay two weeks in advance should the need for two weeks of takehomes arise. For my husband, that means shelling out $224. For patients at other clinics, the price can vary in either direction, but not typically by much.
My husband’s experience highlights another concern facing patients on these medications. For some, extended scripts mean more money up front. Some methadone patients who pay out of pocket are only able to do so daily, relying on cash tips or weekly paychecks to pay for their medicine. Buprenorphine patients who are used to paying for one or two weeks at a time might not have additional funds for a month-long script. Patients whose medications are covered by grants or insurance sometimes have caps on the amount of doses that can be covered at one time, leaving them to pay out of pocket for extra doses. If they can’t pay, clinics are not required to dose them.
Because buprenorphine prescribing is not burdened with as many stringent regulations as methadone, it is easier for providers to adhere to social distancing recommendations while still keeping patients appropriately medicated. Many providers have reverted to telehealth. On March 17, the Secretary of Health and Human Services lifted restrictions on telemedicine practices that prevented Medicare patients from engaging by using cell phones in homes or shelters. On the same day, the Drug Enforcement Administration also waived requirements that patients starting on buprenorphine have an initial in-person visit, temporarily allowing new buprenorphine patients to engage via telemedicine from the start.
But even with these changes, economically disenfranchised patients may struggle to utilize telehealth options. “Not all of my patients have the right smartphones to do telehealth, or the minutes. When I asked them about doing telehealth, they said no way,” said Waldman.
Like Talbott stressed, the response to this crisis is going to vary between states and clinics, with wide discretion placed in the hands of prescribers and medical directors. It is a situation that is changing by the day, as states and counties continue to evaluate the impact of COVID-19 in their communities and how they wish to respond.
“I think my biggest duty right now is to reassure patients that they will not be abandoned,” said Burson.
Correction: An earlier version of this articles stated that all registered nurses were able to prescribe buprenorphine. Only advance practice registered nurses can prescribe that medication.